Everyday Mindfulness for OCD: Tips, Tricks and Skills for Living Joyfully
By Jon Hershfield and Shala Nicely
Written by two clinicians who are honest about having their own personal struggles with Obsessive Compulsive Disorder, Everyday Mindfulness for OCD offers a unique perspective on strategies for staying one step ahead of OCD symptoms. As the title implies, the authors present tips not for just living despite OCD, but for living joyfully with OCD.
This book is not an introductory manual for OCD, instead filling a need for those who are further along in their treatment. It is tailored towards those who already have a solid understanding of OCD and exposure and response prevention, but are looking for more ideas to increase or maintain progress long-term. It may be helpful as a supplement to therapy, or as a secondary book for those who have already completed a self help treatment workbook.
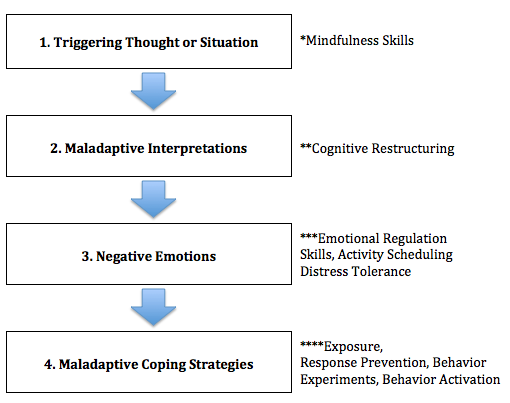
Everyday Mindfulness for OCD is divided into three sections: mindfulness and self compassion, daily tools and games to promote joyful living, and long-term mastery over OCD. The strategies presented feel very practical and concrete. The authors’ suggestions regarding self-compassion seem especially useful, as self-compassion skills can be difficult to develop, yet essential to living a joyful life. There are also a variety of exposure games included, which offer a great way to mix up your ERP practice.
How to Get Help for Obsessive Compulsive Disorder in San Jose/Los Gatos and Sacramento/Roseville
The Cognitive Behavior Therapy Center specializes in therapy and counseling with adults, children and teenagers. Click to send an email for more information on how we can help you or your family members improve your outlook.
Silicon Valley and Sacramento Valley Communities We Serve
Cognitive Behavior Therapy Center of Silicon Valley offers evidence-based therapy for Anxiety and Obsessive Compulsive Disorder near the following Silicon Valley/San Jose communities:
San Jose Therapy Counseling • Saratoga Therapy Counseling • Los Gatos Therapy Counseling • Monte Sereno Therapy Counseling • Cupertino Therapy Counseling • Campbell Therapy Counseling • Mountain View Therapy Counseling • Los Altos Therapy Counseling • Sunnyvale Therapy Counseling • Santa Clara Therapy Counseling
Cognitive Behavior Therapy Center of Sacramento Valley offers evidence-based therapy for Anxiety and Obsessive Compulsive Disorder (OCD) near the following Sacramento Valley and Sierra communities:
Sacramento Therapy Counseling • Roseville Therapy Counseling • Rocklin Therapy Counseling • Granite Bay Therapy Counseling • Lincoln Therapy Counseling • Folsom Therapy Counseling • Citrus Heights Therapy Counseling • El Dorado Hills Therapy Counseling • Loomis Therapy Counseling • Grass Valley Therapy Counseling • Auburn Therapy Counseling
CONTACT US
Click to send an email